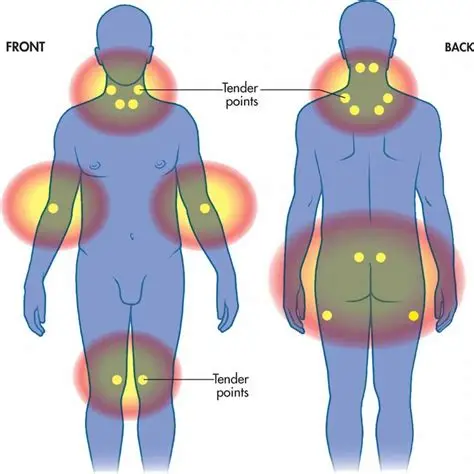
Fibromyalgia is a complex, often misunderstood condition, and many people feel they don’t get the full picture during short medical visits. Here’s a deeper, more practical look at what often goes unsaid—written clearly and directly.
Fibromyalgia is not “just pain.”
It is a disorder of how the brain and nervous system process pain signals. This is called central sensitization, meaning your body amplifies sensations that others might not even notice.
Your pain is real—even if tests are normal.
Blood tests, X-rays, and scans often come back normal. That does not mean nothing is wrong. Fibromyalgia affects function, not structure.
It can affect much more than muscles.
You may experience fatigue, sleep problems, memory issues (“fibro fog”), headaches, and digestive problems like irritable bowel syndrome.
Fatigue can be as disabling as pain.
Many people say exhaustion is their worst symptom. It is not just being tired—it is a deep, unrefreshing fatigue.
Sleep problems are central to the condition.
Even if you sleep for many hours, your body may not reach deep restorative sleep. This worsens pain and fatigue.
Stress plays a major role.
Emotional or physical stress can trigger flare-ups. The nervous system becomes overactive and more sensitive.
There is no single cause.
Fibromyalgia likely results from a mix of genetics, trauma, infections, and long-term stress.
It often overlaps with other conditions.
Common overlaps include chronic fatigue syndrome, migraines, anxiety, depression, and irritable bowel syndrome.
Exercise helps—but feels hard at first.
Gentle, gradual movement like walking, stretching, or swimming can reduce symptoms over time. Starting too intensely can worsen pain.
Medications are only part of the solution.
Drugs may reduce symptoms, but they rarely fix everything. Lifestyle changes are equally important.
Not all medications work for everyone.
Common options include certain antidepressants and nerve pain drugs, but responses vary widely.
Painkillers are often ineffective.
Traditional pain relievers like opioids usually do not work well and may cause harm over time.
Mental health support is important.
This does not mean the illness is “in your head.” Therapy can help manage stress and coping strategies.
Fibro fog is real.
You may struggle with memory, concentration, and word-finding. This is a recognized symptom, not laziness.
Weather and environment can affect symptoms.
Cold, humidity, or sudden weather changes may trigger flare-ups.
Pacing is crucial.
Doing too much on good days can lead to worse symptoms later. Balance activity and rest carefully.
Diet may influence symptoms.
Some people feel better reducing processed foods, sugar, or certain triggers, though no single diet works for all.
Caffeine and sleep don’t mix well.
Too much caffeine can worsen sleep quality, which increases symptoms.
Support systems matter.
Family and friends may not understand your condition. Education and communication help.
You may look “fine” but feel awful.
Fibromyalgia is an invisible illness, which can lead to misunderstanding or disbelief from others.
Diagnosis can take years.
Many people are misdiagnosed or dismissed before receiving proper recognition.
Doctors may disagree on treatment.
Because fibromyalgia is complex, different doctors may suggest different approaches.
Flare-ups are unpredictable.
Symptoms can worsen without a clear reason, making planning difficult.
Small habits make a big difference.
Regular sleep, light exercise, stress management, and routine can improve quality of life.
There is no quick cure—but improvement is possible.
Many people find ways to manage symptoms and live meaningful lives.
You are not alone.
Millions of people worldwide live with fibromyalgia.
Self-advocacy is important.
You may need to speak up about your symptoms and what helps you.
Tracking symptoms can help.
Keeping a journal may reveal patterns and triggers.
Alternative therapies may help some people.
Options like acupuncture, massage, or yoga can provide relief for certain individuals.
Hydration and nutrition matter.
Simple basics like drinking enough water and eating balanced meals support overall health.
Hormones can influence symptoms.
Some people notice changes during menstrual cycles or menopause.
Overexertion is a common mistake.
Pushing through pain often leads to worse symptoms later.
Rest is necessary—but too much rest can worsen stiffness.
Balance is key.
You may need to redefine productivity.
Living with fibromyalgia often requires adjusting expectations and priorities.
Work and daily life may need modification.
Flexible schedules or reduced workload can help.
Pain does not always reflect damage.
Your nervous system may signal pain even without injury.
Education empowers you.
Understanding your condition helps you manage it better.
Progress is often slow.
Improvement happens gradually, not overnight.
Good days and bad days are normal.
Fluctuation is part of the condition.
Comparing yourself to others can be harmful.
Each person’s experience is different.
Acceptance can reduce stress.
Fighting the condition mentally can increase tension and symptoms.
You deserve to be taken seriously.
Your experience is valid.
With the right combination of strategies—medical care, lifestyle changes, and support—many people with fibromyalgia build stable, fulfilling lives despite the challenges.
What Your Doctor May Not Tell You About Fibromyalgia